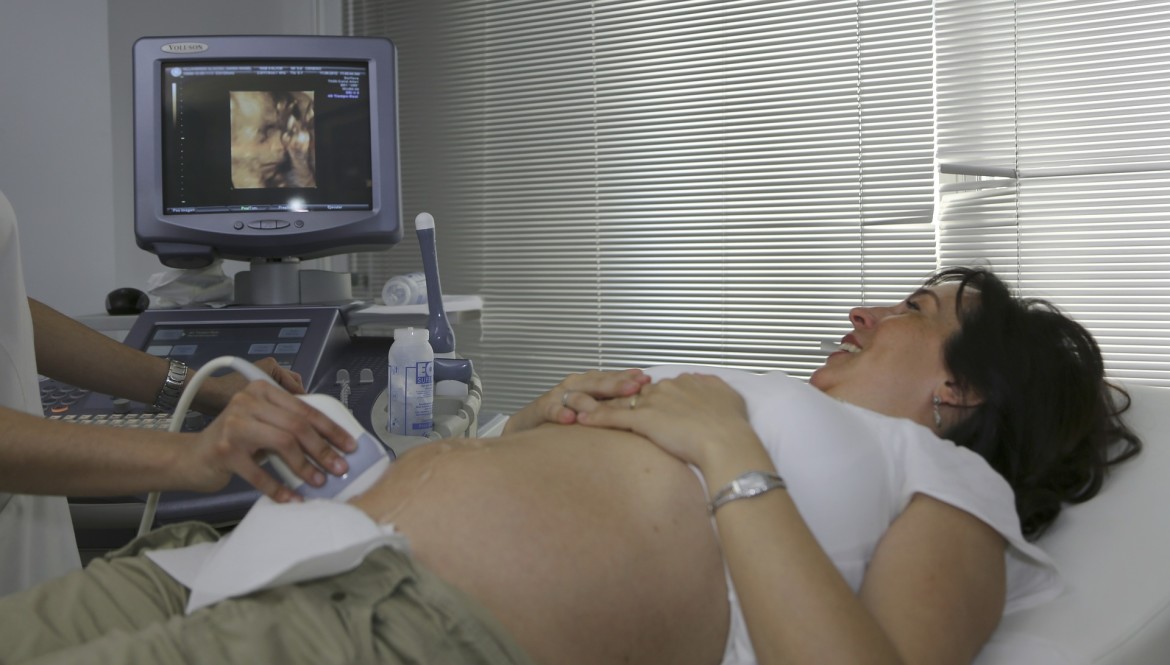
The risks and benefits of ultrasounds in pregnancy
21 Oct, 2019As new technologies become available, there seems to be a trend where they are used widely prior to testing. For example, x-rays of babies in utero were performed until they realised that there was an increase in cancer among the children who were x-rayed in their mothers uterus as foetus’. Similarly, Thadilomide was introduced in the 1940s and people used it commonly after WWII for sleeplessness. It was marketed as being completely safe in pregnancy but it was later found that it caused phocomelia in children whose mothers consumed the drug whilst pregnant. These children were born with shortened, missing or flipper like limbs. As such, many other procedures, medications and other uses for technology have been integrated into normal practice and routines today that should be questioned and an informed decision made by the parents on whether to proceed with it or not.
Ultrasound scanning
Ultrasound scanning was introduced to scan the foetus for abnormalities and become widely used in the 1970s. A scottish obstetrician used an industrial ultrasound for detecting flaws in metal and used it on pregnant women and by the 1980s it became routine in many countries.
In Ina May’s Guide to Childbirth, she states that the use of ultrasound is especially unregulated and popular in the United States. The FDA has relinquished control over the amount of sonic energy that can be emitted by ultrasound devices in obstetrics. There are also no federal or state regulations requiring calibration of the ultrasound machines on a periodic basis, indications for the procedure, type of equipment, amount of exposure, ID or qualifications of sonographer. Basically, anyone can buy an ultrasound device and use it on a pregnant woman.
To me it seems shocking that machines used in manufacturing, production, weighing scales in the supermarket all need to be calibrated and checked biannually, and most ultrasound machines only need to be calibrated on a periodic basis to be accredited.
Ultrasounds for diagnostic screening
An ultrasound is useful to diagnose the following:
If the fetus is alive
The age of the fetus (if early pregnancy)
How many babies there are
The location of the placenta
The position of the baby
Growth rate of the baby (by comparing scans done two weeks apart)
The sex of the baby - a guess, but could be incorrect
All of the above can usually be identified through other means if required, or in the case of sex of the baby, need not be known until its born. It definitely helps parents feel more secure to know some of this information through an ultrasound, and informed, but doesn’t improve outcomes for the mother or child in any way.
For example, a mother can usually tell if the fetus is alive through kicking, hearing its heartbeat through a fetoscope. A good midwife will be able to feel the uterus and feel two different babies in there in the case of multiple babies, and be able to identify the position of the baby closer to term. If you are eating well then your baby’s growth rate will be fine and if there are issues, such as a kink in the umbilical cord for example, moving around can usually resolve this. The location of the placenta can be worrying in the case of placenta praevia, however knowing this during pregnancy doesn’t really help. If the placenta is blocking the baby from descent during labour, then an emergency c-section will need to be performed. As for the baby’s due date, you may be able to use accurate records of your period, temperature charts and the baby’s size. Ultrasounds have been known to be as much as 5 pounds off when estimating the baby’s weight so its by no means an accurate measure of weight to then figure out how far along you are and estimate the due date.
If your doctor or midwife asks you to have an ultrasound, and you would prefer not to have one, ask them why they would like you to do one, and what specific information they want from it. There is usually another way to get this information as described above.
Ultrasounds to assess pelvic dimensions
Ultrasounds can also be used by doctors to measure the mothers pelvic dimensions. This is another piece of information that can be gained without the use of ultrasound technology. The midwives at the farm use their hand to make this judgement rather than ultrasounds and find that its a much better estimation. Ina May Gaskin states in Ina May’s Guide to childbirth that she had 25 women come to them who were told by their doctors that their pelvises were ‘inadequate’, that is too small for a normal birth. Except for two women, all other women were able to give birth vaginally. Through practice and experience, the Farm midwives are able to feel the size of the baby and instinctively know whether the mother’s pelvis is large enough for it to come through.
Additionally, the position you are in in labour will change the width of your pelvis. When you’re getting an ultrasound you are flat on your back which will change the position of your pelvis. But the pelvis is not fixed in size which is something not a lot of doctors know. The pelvis is made up of four separate bones connected with ligaments. In the late stages of pregnancy, your body will produce the hormone relaxin which loosens these ligaments, allowing the pelvic cavity to grow wider. The width of your pelvis on your back is much smaller than when you are on your hands and knees. Similarly, you can use knee positions on the floor to widen the passage at different parts depending on where the baby is stuck. For example, if the baby’s head is stuck near the top of the passage, you can get on all fours, with your knees spread apart and ankles placed together. Once it is through this part of the pelvis, then move your knees together and ankles spread out at 45 degree angles, this will widen the lower part of the pelvic cavity and allow the head to move lower.
Research on Safety of Ultrasounds for Prenatal scans
In the short term no problems have been identified with ultrasound use although it has been used so much, but they haven’t been around long enough to do any long-term studies on the hazards of using ultrasounds in pregnancy. Medicine has no studies or research on the long term effects of ultrasounds yet they are continued to be used widely in most practices.
https://www.ncbi.nlm.nih.gov/pubmed/12071478
This article in the Epidemiology journal suggests that a conference should be held to gather data and provide guidelines for future research that should take place, seeing as there have been reported effects of growth restriction, delayed speech, dyslexia and non-right handedness associated with ultrasound exposure. Whilst there are no conclusive studies that there is an impact, neither are there studies that there is no impact. It also suggests the studies should measure the ‘acoustic output, exposure time, number of exposures per subject, and the timing during pregnancy when the exposure occurred’. Considering how widespread the use of ultrasounds are for prenatal scans, its surprising that there are no long term in-depth studies performed to date. The continued use is not defined as a trial either, meaning that it can be used as part of normal practice almost anywhere.
https://www.ncbi.nlm.nih.gov/pubmed/24176149
Another article states that ultrasound is one of the most commonly used diagnostic procedures in obstetrics and is widely believed to be safe. There is a general belief that it does not pose any risk to the mother or foetus. The study does state though that ultrasounds are a form of energy and affects biological tissue through thermal or non-thermal mechanisms. At present it has not been determined whether these bioeffects are harmful. The study suggests that it is the role of since to provide this information and perhaps perform a risk benefit analysis, and educate users of ultrasound to provide information for patient safety.
https://obgyn.onlinelibrary.wiley.com/doi/pdf/10.1576/toag.8.4.222.27271
This article explores literature on long term and short term effects of ultrasounds and concludes that while there is no significant evidence of an affect on mother or child, the risks are around consistency in use with minimum possible acoustic power output, duration and exposure, and awareness of safety and prudent use is imperative. It also says that the greatest risk of danger to the fetus is misdiagnosis. The report also has a section on long term effects and references some of the studies mentioned in the NCBI article in the Epidemiology Journal referred to earlier e.g. reports of dyslexia, speech delay, intrauterine growth restriction and low birthweight. There was however another study done on all the epidemiological evidence which found that there was no correlation between ultrasound use and low birth weight, neurodevelopment issues or childhood malignancies. It concludes that “While these findings are reassuring and, at present, the general consensus is that diagnostic ultrasound is safe in pregnancy, with no substantiated long-term effects, caution should, nonetheless, be exercised as machines become ever more powerful.”
This petition on change.org is signed by a number of high profile doctors demanding more research and regulation on Ultrasounds. It refers to other research and studies performed which are really useful. There are a number of alarming points in here, which I will try to summarise:
There is no consistent way of knowing how much ultrasound is used during a scan session as this is not required to be recorded. This means that researchers can’t look at ultrasound dosage and compare with health outcomes. There are correlations between groups that receive a higher number of ultrasounds and health conditions such as autism. Refer to the work of Dr. David Toms, and www.ultrasound-autism.org
Almost half of all medical ultrasound units out there in clinics are defective. This may result in a worse picture, requiring extra exposure to make a diagnosis. Ultrasound machines require more frequent maintenance. It also states that annual calibration is not sufficient. https://www.ncbi.nlm.nih.gov/pubmed/18945726 and https://academic.oup.com/ehjcimaging/article/11/9/801/2396954
The average number of ultrasounds varies between a healthy pregnancy (4) to a high risk pregnancy (20 or more). There is no consistency in skill of sonographers and therefore how much ultrasound they use. There is also a growing trend of clinics offering hour long ultrasound recordings for mementos of the pregnancy which is an unnecessary risk. https://www.researchgate.net/publication/40846908_Proliferation_of_prenatal_ultrasonography
https://chriskresser.com/natural-childbirth-iib-ultrasound-not-as-safe-as-commonly-thought/
This article discusses some of the risks in ultrasound use, looking at studies on animals also retrospective studies on human babies. It found a number of worrying results especially in relation to the Doppler Ultrasound which reported results of intrauterine growth restrictions, another study in the UK found that babies who had had 2 or more scans had 2 times the risk of perinatal death. Another study of 72 children found that a child with delayed speech was twice as likely to have been exposed to an ultrasound. On the other hand there was a review by the WHO in 2009 and another review in 2008 which suggested that ultrasounds are safe and have no impact other than potentially causing non-right handedness in males due to disruption to the fetal brain.
The author of this article suggests three steps in minimising ultrasound use:
Using ultrasound only when medically indicated, i.e. only when a problem is suspected, rather than as a routine screening to determine the sex of the baby or check on its development.
Minimize total exposure time (by choosing a skilled and knowledgeable operator).
Minimize exposure intensity (i.e. avoiding Doppler during the first trimester especially).
Conclusion
I will leave you to make your own conclusions on whether you would be willing to get an ultrasound of your baby in utero. Have a think about the benefits - what information are you likely to get from it, and is this information likely to be reliable. Think about the potential risks, including misdiagnosis, and how this may affect decisions you will make and your emotional health during the pregnancy, and make an informed decision based on the facts - or lack thereof in the case of ultrasounds, since there have been no long term studies.
Cover Image by Medical Prudens from Pixabay
Get The Best Of Sleepy Roo Delivered To Your Inbox
Subscribe to my newsletter and get the latest info on baby sleep! You can unsubscribe at any time.